Science
Henrietta Lacks’s Cells Revolutionize Medical Research and Ethics

Seventy-five years ago, Henrietta Lacks unknowingly became a pivotal figure in medical history. In 1951, doctors at Johns Hopkins Hospital harvested cells from Lacks, an African American patient suffering from cervical cancer, without her consent. These cells, known as HeLa cells, became instrumental in numerous medical breakthroughs, including the development of vaccines for polio and HPV, as well as treatments for HIV/AIDS, leukemia, and influenza. Although Lacks passed away in 1951, the influence of her immortal cells continues to shape research and ethical standards in the field.
The significance of HeLa cells is being reflected upon by researchers worldwide. Dr. Cigall Kadoch, an associate professor of pediatric oncology at Dana-Farber Cancer Institute and Harvard Medical School, remarked that the existence of an immortalized cell line derived from a patient unaware of its extraction is remarkable. “To the modern researcher, the fact that cells were taken and established into an immortalized, forever-growing cell line from a patient that didn’t know that happened is astounding,” Kadoch stated.
Lacks’s story gained notoriety following the publication of Rebecca Skloot‘s book, “The Immortal Life of Henrietta Lacks,” in 2010. Recently, Lacks’s family filed a lawsuit against Waltham-based Thermo Fisher Scientific, claiming the company profited billions from the unethical practices of a racially biased medical system. In 2023, her descendants reached a confidential settlement with the biotechnology firm, along with a similar agreement with Novartis earlier this month.
Born in 1920 in Roanoke, Virginia, Lacks worked on a tobacco farm before marrying David “Day” Lacks in 1941 and having five children. Her first visit to Johns Hopkins was on February 1, 1951, where she reported a “knot” in her cervix. The hospital was among the few at the time offering public medical care for Black patients. Unfortunately, it was common practice for hospitals to use public ward patients for research without their consent.
After being diagnosed with cervical cancer, Lacks signed a consent form for any necessary operations, unaware that samples from both her tumor and healthy cervical tissue would be collected. These samples were sent to Dr. George Gey for culturing in his laboratory. Remarkably, Lacks’s cells were labeled “HeLa,” derived from the first two letters of her first and last names. Unlike previous attempts, Gey found that Lacks’s cancerous cells thrived and multiplied rapidly outside the human body.
Dr. Sabrina Assoumou, an infectious disease physician at Boston Medical Center, credits much of her research on HIV to the foundational work involving HeLa cells. Assoumou is currently engaged in disseminating a long-acting HIV medication called Sunlenca, approved by the FDA. She emphasizes the importance of making this treatment accessible to marginalized communities. “HeLa cells have been really critical for many scientific discoveries, especially for HIV,” Assoumou explained.
Research has shown that HeLa cells do not become infected with HIV in the same manner as immune cells. Scientists have manipulated the DNA of HeLa samples to study how HIV affects cells, leading to advancements in treatment options. “Understanding the mechanisms helped us later develop drugs that enable me to help my patients live longer and happier lives,” Assoumou noted.
Kadoch’s research at Dana-Farber utilizes HeLa cells to explore the genetic underpinnings of various cancers. She highlights the diversity of cancer types and stresses the need for comprehensive research approaches. “Cancer is not one disease, but a very diverse, heterogeneous collection of many different diseases,” Kadoch stated. The challenge, she noted, lies in the variability of cell lines cultured in different lab environments, as “no two HeLa cell lines from two different labs are the same.”
The legacy of HeLa cells extends beyond scientific advancements; it has prompted a reexamination of ethical standards in research. Assoumou has contributed to a course at Boston Medical Center aimed at educating medical interpreters on the historical context of medical mistrust, including the experiences of Lacks and the infamous Tuskegee syphilis study. The course aims to empower interpreters to advocate for patients who may face language barriers.
“We’ve learned and developed procedures and practices to help us be better researchers,” Assoumou said. Kadoch concurs that informed consent is vital for ensuring diversity among research participants. “We’ll do a better job for our worldly effort against cancer if we understand the heterogeneous repertoire of individuals that get these diseases,” she added.
Kadoch believes many researchers are still unaware of the full story behind HeLa cells. She emphasizes the importance of recognizing the contributions of patients like Lacks in scientific research. “Know what you work with, and where it came from,” she advised.
Henrietta Lacks’s cells have not only transformed medical research but also catalyzed essential conversations about ethics and consent in the scientific community. As researchers continue to build upon her legacy, the importance of informed consent and the recognition of all contributors to science remain paramount.
-
 Science4 months ago
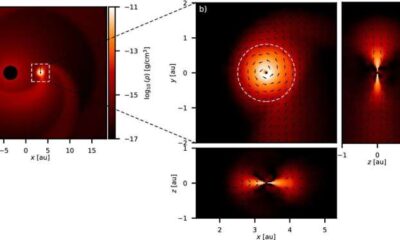
Science4 months agoALMA Discovers Companion Orbiting Giant Star π 1 Gruis
-

 World4 months ago
World4 months agoF-22 Raptor vs. Su-57 Felon: A 2025 Fighter Jet Comparison
-

 Science4 months ago
Science4 months agoUniversity of Hawaiʻi Joins $25.6M AI Project for Disaster Monitoring
-

 Science4 months ago
Science4 months agoInnovator Captures Light at 2 Billion Frames Per Second
-
 Science4 months ago
Science4 months agoOhio State Study Uncovers Brain Connectivity and Function Links
-

 Politics2 months ago
Politics2 months agoU.S. Visa Rescheduling Hits H‐1B Applicants as New Vetting Rules Take Effect
-

 Politics4 months ago
Politics4 months agoHamas Chief Stresses Disarmament Tied to Occupation’s End
-

 Entertainment4 months ago
Entertainment4 months agoMegan Thee Stallion Exposes Alleged Online Attack by Bots
-

 Entertainment4 months ago
Entertainment4 months agoPaloma Elsesser Shines at LA Event with Iconic Slicked-Back Bun
-

 Science5 months ago
Science5 months agoResearchers Challenge 200-Year-Old Physics Principle with Atomic Engines
-

 World4 months ago
World4 months agoFDA Unveils Plan to Cut Drug Prices and Boost Biosimilars
-

 Entertainment4 months ago
Entertainment4 months agoBeloved Artist and Community Leader Gloria Rosencrants Passes Away








